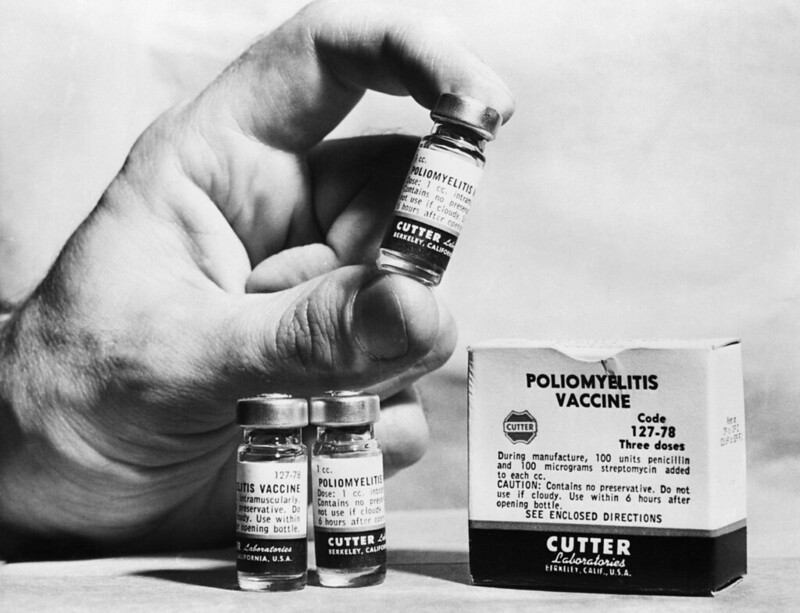
Photo courtesy of Tullio Saba
Polio is on the short list of infectious diseases with the potential to be completely eradicated from the globe, with smallpox and rinderpest being the only two eradicated diseases to date. The Global Polio Eradication Initiative has worked to vaccinate nearly 3 billion children for polio around the globe since it was launched in 1988.1 This effort has led to a 99% decrease in polio incidence, and wild poliovirus is now only endemic in two countries: Pakistan and Afghanistan.1 While this global effort has proven successful, polio still poses a threat in communities that have low levels of vaccination uptake, and the potential for vaccine-derived polio cases remains present. The recent detection of poliovirus in London sewage surveillance samples has sparked concern for the virus that has not been a cause of concern in the United Kingdom (UK) for many years.2
Polio is a viral infection caused by poliovirus. The vast majority of poliovirus infections are asymptomatic, while about 25% of those infected will develop flu-like symptoms that often resolve on their own within 2-5 days.3 Less than 1% of cases will develop more severe symptoms, including paralysis, and be classified as paralytic polio.3 The CDC estimates that the case fatality rate of paralytic polio is 2-5% among children and up to 15-30% among adults.4 The virus spreads through contact with contaminated stool and bodily fluids, such as a sneeze.5
While there is no known cure for polio, two vaccines are available to prevent the virus: inactivated poliovirus vaccine (IPV) and oral poliovirus vaccine (OPV).3 Both vaccines are 99%-100% effective at preventing the virus if given in the full series of recommended doses.6 OPV includes a very small amount of weakened poliovirus, which on rare occasion can lead to vaccine-derived polio (VDP) infection in someone who is unvaccinated.5 In this situation, the weakened poliovirus in the oral vaccine can adapt to behave more similarly to wildtype poliovirus and spread more easily from the person who received an OPV to an unvaccinated person who comes in contact with their feces or bodily fluid. Vaccine-derived poliovirus is rare, with under 760 cases occurring worldwide since the year 2000, while over 10 billion doses of oral polio vaccine have been administered in the same timeframe.7 The United States and UK use IPV to vaccinate their populations in an effort to prevent VDP infection; however oral vaccines are still commonly used in many countries around the world.5 Both types of vaccines prevent both wild type poliovirus as well as vaccine-derived poliovirus infections, so if a population is fully vaccinated they are protected from all forms of the virus. However, if members of a community are unvaccinated for polio, they can contract the virus from someone who recently got the OPV. This is the likely explanation for the poliovirus that has been detected in the London sewer.2
The last case of wild poliovirus reported in the UK was detected almost 40 years ago in 1984.2 London has been doing routine sewage surveillance for polio since the early 2000s, and it is typical for the surveillance system to detect poliovirus around 1-3 times in any given the year.8 These occasional and independent detections of virus are not generally a cause for concern of community spread, but rather an indication that someone in the community has received the oral polio vaccine while visiting a country where they are commonly administered. However, in this case, the virus has been detected more consistently in the sewage system from February to June of this year which suggest the potential for an outbreak.2 Although there have been no reported cases of polio infection as of mid-July, UK health officials have classified the virus as vaccine-derived, and believe the virus could be spreading among a small community of people in London.2 As a result of the poliovirus detection, the UK health department is further investigating the reports of virus, and wastewater surveillance is being expanded in the area to better assess where the virus originated from and where it is potentially spreading.2 London residents are encouraged to check their child’s polio vaccination status to make sure they are up to date with the vaccine.2 While the threat of poliovirus spreading widely among the general public in London is low, it is still important for residents to make sure they are up to date with vaccination. Prevention is key, as there is currently no treatment for polio.
Until eradication efforts are successful world-wide, poliovirus will continue to be detected in many countries. Israel faced similar circumstances in March of this year, with multiple reports of polio virus detected in the sewage surveillance system which prompted widespread vaccination efforts.9 Mozambique and Malawi have also experienced polio outbreaks this year; however those outbreaks consisted of the wild type poliovirus rather than vaccine derived poliovirus.10 The continuation of polio eradication efforts is needed to prevent further outbreaks in London, Israel, Africa, and beyond.
References
- https://www.gatesfoundation.org/our-work/programs/global-development/polio#:~:text=In%201988%2C%20when%20the%20Global,by%2099%20percent%20since%20then.
- https://www.gov.uk/government/news/poliovirus-detected-in-sewage-from-north-and-east-london
- https://www.cdc.gov/polio/what-is-polio/index.htm
- https://www.cdc.gov/vaccines/pubs/pinkbook/polio.html#:~:text=The%20case%20fatality%20ratio%20for,to%2075%25%20with%20bulbar%20involvement.
- https://www.cdc.gov/vaccines/vpd/polio/hcp/vaccine-derived-poliovirus-faq.html#:~:text=What%20is%20a%20vaccine%2Dderived,wild%20or%20naturally%20occurring%20virus.
- https://www.cdc.gov/vaccines/vpd/polio/hcp/effectiveness-duration-protection.html#:~:text=Two%20doses%20of%20inactivated%20polio,of%20IPV%20and%20tOPV%2C%20or
- https://www.who.int/news-room/questions-and-answers/item/poliomyelitis-vaccine-derived-polio
- https://www.science.org/content/article/poliovirus-in-london-sewage-sparks-alarm
- https://www.who.int/emergencies/disease-outbreak-news/item/2022-DON366
- https://news.un.org/en/story/2022/05/1118502